
Quick Guide to Non-Drug CRPS Treatments
Key Takeaways:
- Desensitization retrains skin sensitivity using texture progression.
- Graded Motor Imagery (GMI) fixes brain map distortions through three stages.
- Evidence shows 50-70% improvement when started early (within one year).
- Consistency is critical; daily short sessions beat occasional long ones.
- Specialist training prevents symptom worsening during therapy.
Living with Complex Regional Pain Syndrome (CRPS) often feels like being trapped in a malfunctioning alarm system. Your body screams danger when there is no threat. Standard painkillers often miss the mark because the problem isn't just the tissue; it's how your nervous system processes signals. While medication plays a role, the real game-changer lies in non-drug approaches that retrain your brain. Specifically, Desensitization Therapy A systematic process exposing the affected limb to varying textures to reduce hypersensitivity. and Graded Motor Imagery (GMI) A cognitive rehabilitation protocol involving left/right discrimination, motor imagery, and mirror therapy. stand out as the most effective tools available today. These methods don't just mask symptoms; they attempt to reverse the neurological changes causing them.
Understanding Desensitization: Retraining the Senses
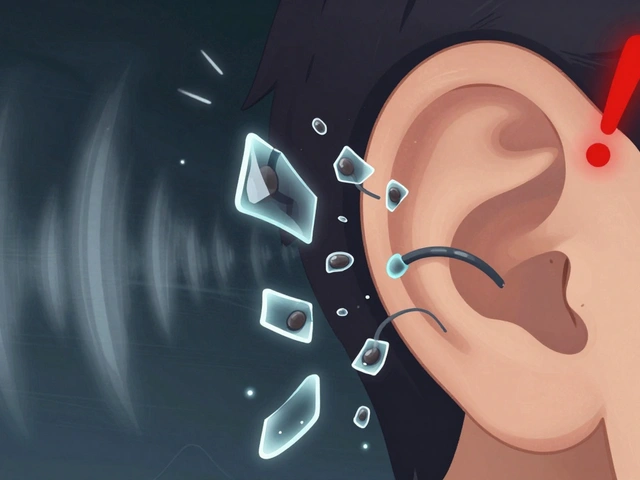
Many people assume pain comes from a damaged area, so they avoid touching it. In CRPS, avoidance actually reinforces the pain signal. Desensitization therapy flips this script by gently teaching your skin that touch is safe again. This isn't about rubbing raw skin until it hurts. It is a slow, graduated process designed to normalize activity in the dorsal horn neurons of your spinal cord.
The goal is to manage cutaneous hypersensitivity-where even a sheet feels like sandpaper. According to clinical guidelines from the American Occupational Therapy Association, you start with materials lighter than air. Think cotton balls or silk fabric applying less than 10 grams of pressure. You hold this contact for short bursts, typically five minutes, three times a day. The magic happens when you measure progress. Using the Visual Analogue Scale (VAS), you track your pain score during these sessions. You only move to the next texture, like soft wool, once your pain stays below a 3 out of 10 during the activity.
Over four to twelve weeks, the textures change. Cotton gives way to velvet, then denim, eventually leading to normal clothing contact. A randomized controlled trial published in Pain Medicine (2021) showed that patients following this structured protocol improved their functional scores by 42% more than those receiving standard care. However, patience is vital. Pushing too fast can trigger a flare-up. If your hand temperature rises significantly or color changes happen, step back to the previous texture level immediately.

Decoding Graded Motor Imagery (GMI)
If desensitization calms the skin, Graded Motor Imagery repairs the map in your head. Research suggests that in CRPS patients, the representation of the affected limb in the Somatosensory Cortex The part of the brain responsible for processing sensory information from the body. gets "smudged" or disorganized. Neighboring areas expand into the space meant for the hurt limb. Dr. G. Lorimer Moseley pioneered this approach, proving that mental exercises can physically reshape this brain map.
GMI follows three distinct stages, acting like stepping stones across a river. Skipping steps usually results in failure. Stage one focuses on Left/Right Discrimination. You show yourself pictures of hands (or feet) moving quickly. Your job is simply to say which hand is shown. You use apps like Recognise Online for this. The goal is speed and accuracy-aim for 90% correct identification within 1.5 seconds per image. It sounds easy until you're doing 50 images daily. This task forces the brain to engage visual-spatial areas associated with movement without triggering pain receptors.
Once discrimination accuracy stabilizes, you move to explicit motor imagery. Here, you mentally rehearse moving your limb without actually lifting it. Imagine bending your wrist or wiggling fingers. Start with five minutes daily. By week six, extend to 20 minutes. Finally, Stage three introduces Mirror Therapy Using a reflective surface to create a visual illusion that the affected limb is moving pain-free.. This uses a mirror box placed vertically between your limbs. When you move the healthy limb, its reflection hides the affected limb. Your brain sees the "sick" limb moving normally. A landmark study in Brain (2006) found 70% of participants saw a 50% drop in pain after just four weeks of this combination protocol.
The Science Behind Success Rates
You might wonder if this is just placebo. The data suggests otherwise. National guidelines updated in 2023 recommend these techniques as first-line treatments. Success relies heavily on timing. The Cleveland Clinic reports an 83% success rate when therapy begins within three months of symptom onset. This drops to 42% if you wait longer than 12 months. Early intervention capitalizes on higher neuroplasticity-the brain's ability to rewire itself before maladaptive pathways become rigid.
We look at hard metrics, not just feelings. The Disabilities of the Arm, Shoulder and Hand (DASH) questionnaire measures function better than vague descriptions. Patients undergoing combined multimodal therapy-mixing GMI, desensitization, and sometimes psychological support-see a 5.2-point reduction on the 10-point Numerical Pain Rating Scale over 24 weeks. Compare this to traditional range-of-motion exercise alone, which yields only about a 1.5-point drop. The difference is massive for daily life. That extra 3.7 points could mean the difference between sleeping through the night or waking every hour.

Implementing Therapy Safely at Home
While professional guidance is ideal, many protocols can be adapted for home practice under supervision. The NOI Group recommends daily sessions of 15 to 20 minutes rather than sporadic marathon sessions. Consistency rewires circuits faster than intensity. However, safety checks are mandatory. Only therapists with specialized training-like Certified Hand Therapists (CHT)-should direct your program initially. Improper implementation accounts for 22% of treatment failures, according to recent audits. A common mistake involves advancing too quickly. For instance, jumping from cotton ball contact to wearing socks too soon triggers severe flares.
Visual cues help monitor progress. Keep a log tracking duration, texture, and pain scores before and after. If the post-session score is lower or stable, you are on the right track. If it spikes permanently, revert to the previous phase. Digital tools are emerging too. AI-guided apps like Miro Therapeutics now exist, showing 35% better adherence rates compared to paper logs. However, screen time shouldn't replace the physical act of feeling textures or performing imagery exercises.
Real Stories from Recovery Paths
Numbers tell part of the story, but lived experience tells the whole truth. In a survey by the CRPS Patient Foundation (2023), 68% of respondents noted meaningful relief using GMI. One community member shared how their hand temperature normalized from a dangerously cold 82°F to a healthy 96°F after three months. Another noted regaining the ability to wear socks-a small victory for someone who hasn't felt bare skin touch for years. These gains aren't instant miracles. They often come with frustration. About 18% quit due to early difficulty. The first few weeks can be brutal, sometimes spiking pain by 30%. Yet, those who persisted reported breakthroughs around week six.
Beyond personal anecdotes, experts like Dr. Robert Schwartzman view GMI as the single biggest advance in CRPS rehab in the last twenty years. He emphasizes that targeting cortical dysfunction addresses the root cause rather than the symptom. This shift from symptomatic management to restorative neurology marks a turning point in how we view chronic pain conditions globally.
How long does desensitization take to work?
Most patients see initial improvements within 4 to 8 weeks of consistent daily practice. Progress depends on starting textures and sticking to the 3-5 sessions daily recommendation.
Can I do mirror therapy without a special box?
Yes, you can make a DIY mirror box using a cardboard box and a regular mirror, ensuring it blocks the view of the affected limb completely while reflecting the healthy one.
Is GMI suitable for everyone with CRPS?
It works best for those with intact vision and cognition. Patients with severe cognitive impairment (MMSE score below 24) or major visual disturbances may struggle with left/right discrimination tasks.
What indicates I am progressing correctly?
Good progress means pain levels remain stable or decrease slightly after sessions. If pain lingers hours later or worsens significantly, you are likely advancing too fast and should retreat to an easier step.
Does insurance cover these therapies?
Coverage varies by provider. Since 2023, NHS guidelines mandate access to these treatments, but private insurers in the US may require detailed documentation from specialists justifying the necessity.
10 Comments
Amber Armstrong
April 3 2026
It really hits home when you read about the texture progression and how gentle the process needs to be. I remember crying just because a light blanket touched my leg even though there was no actual injury there. The idea of starting with cotton balls feels almost insulting to how raw I felt back then when my skin was hypersensitive. My therapist tried to tell me to go slowly but I was desperate for relief and rushed the timeline. Ending up pushing myself too hard caused weeks of setbacks that could have been easily avoided if I listened. Reading the section about the dorsal horn neurons finally made sense of why the pain felt so electric and uncontainable sometimes. It wasn't just skin sensitivity anymore it was deep in the wiring of my spinal cord and brain connections. Graded Motor Imagery sounds terrifying at first glance for someone who hasn't moved their hand in months without flaring up. But the logic of fixing the brain map before the arm actually moves makes so much theoretical sense to me now. I worry about people quitting during the brutal first few weeks described in the survey data provided here. Frustration is probably the biggest enemy during the three months of trying to normalize limb temperature completely. Seeing the numbers for DASH questionnaire improvements gives a glimmer of hope though for anyone struggling daily. Functional gains are what matter most when you cannot shower without help or hold a cup. We need more resources for home practice so patients do not feel isolated in this journey alone. Consistency truly beats intensity according to every story I have heard from support groups online lately. It feels like we are finally treating the cause instead of just masking the symptom with endless pills forever.
RONALD FOWLER
April 4 2026
Absolutely agree that consistency matters more than duration. Many people rush through stages and fail to see progress. Patience is key.
Biraju Shah
April 4 2026
We need to talk about the risk factors involved in unsupervised mirror therapy. Moving too fast damages the neural pathways we are trying to rebuild. Patients must understand that self diagnosis leads to worse outcomes here.
Cameron Redic
April 4 2026
This sounds promising until you check your deductible and realize nobody covers this nonsense. The claims are overblunded for a therapy that takes months to show minimal results. Save your money.
Marwood Construction
April 5 2026
Regarding insurance coverage, the documentation requirements for private insurers have become significantly more stringent following recent policy updates. Specialists must justify the medical necessity through detailed logs of functional decline prior to approval. The lack of standardization across providers remains a significant barrier to accessible care for chronic pain conditions.
William Rhodes
April 7 2026
You have to fight for your own recovery because no one else is going to do it for you. Neuroplasticity is the ultimate weapon against the disorder if you have the willpower to endure the discomfort. Giving up guarantees failure while persistence forces the brain to adapt regardless of the resistance.
Dan Stoof
April 8 2026
I love the DIY mirror box idea so much!!! It makes the treatment so much more affordable for everyone!!! The cardboard trick is genius!!! I am going to try this immediately!!!
Calvin H
April 10 2026
Right just another miracle cure until insurance denies it again.
Carolyn Kask
April 11 2026
You Americans always complain about costs when our system mandates access to these treatments by law. Your reluctance to pay for preventative neurology shows a fundamental misunderstanding of economic efficiency in healthcare.




Victor Ortiz
April 1 2026
The statistics cited here rely heavily on compliance which is rarely measured accurately in real world settings. Most patients abandon the protocol once the initial novelty wears off and the pain spikes again during the transition phases. You cannot ignore the placebo effect inherent in cognitive therapies lacking pharmacological endpoints. I suspect the success rates drop significantly when removing the specialist supervision element entirely. Home practice introduces variables that ruin the controlled data presented in these papers.