PPI-Clopidogrel Interaction Tool
Find the safest proton pump inhibitor for your clopidogrel therapy
Based on current medical guidelines and interaction research
When you're on clopidogrel after a heart attack or stent placement, your doctor prescribes it to keep your blood from clotting. But if you also have stomach issues - and many do - you might be told to take a proton pump inhibitor (PPI) like omeprazole to protect your gut. Sounds simple, right? Except there's a hidden problem: some PPIs can make clopidogrel less effective. And that could mean the difference between staying safe and having another heart event.
Why Clopidogrel Needs Help to Work
Clopidogrel isn't active when you swallow it. It's a pro-drug that your liver must turn into its active form to block platelets from sticking together. That conversion depends heavily on one enzyme: CYP2C19. If this enzyme is blocked or slowed down, clopidogrel doesn't work as well. And that's where some PPIs come in.Not all PPIs are the same. The problem isn't with PPIs as a group - it's with how they interact with CYP2C19. Omeprazole and its close cousin esomeprazole are strong inhibitors of this enzyme. Studies show they can cut the active metabolite of clopidogrel by up to 49% at high doses. That’s not a small drop. It’s enough to raise the risk of stent clots, heart attacks, and strokes in vulnerable patients.
The PPIs That Cause the Most Trouble
Here’s what the data says about different PPIs and their impact on clopidogrel:| PPI | Effect on Clopidogrel Activation | Clinical Risk |
|---|---|---|
| Omeprazole | Reduces active metabolite by 32-49% | High - FDA black box warning |
| Esomeprazole | Similar to omeprazole | High - Avoided in guidelines |
| Lansoprazole | Reduces by ~25% | Moderate |
| Rabeprazole | Reduces by ~28% (max), no change in overall exposure | Moderate |
| Pantoprazole | Reduces by only 14% (even at high dose) | Low - Preferred alternative |
| Dexlansoprazole | Minimal inhibition | Low - Recommended in 2023 ACC/AHA guidelines |
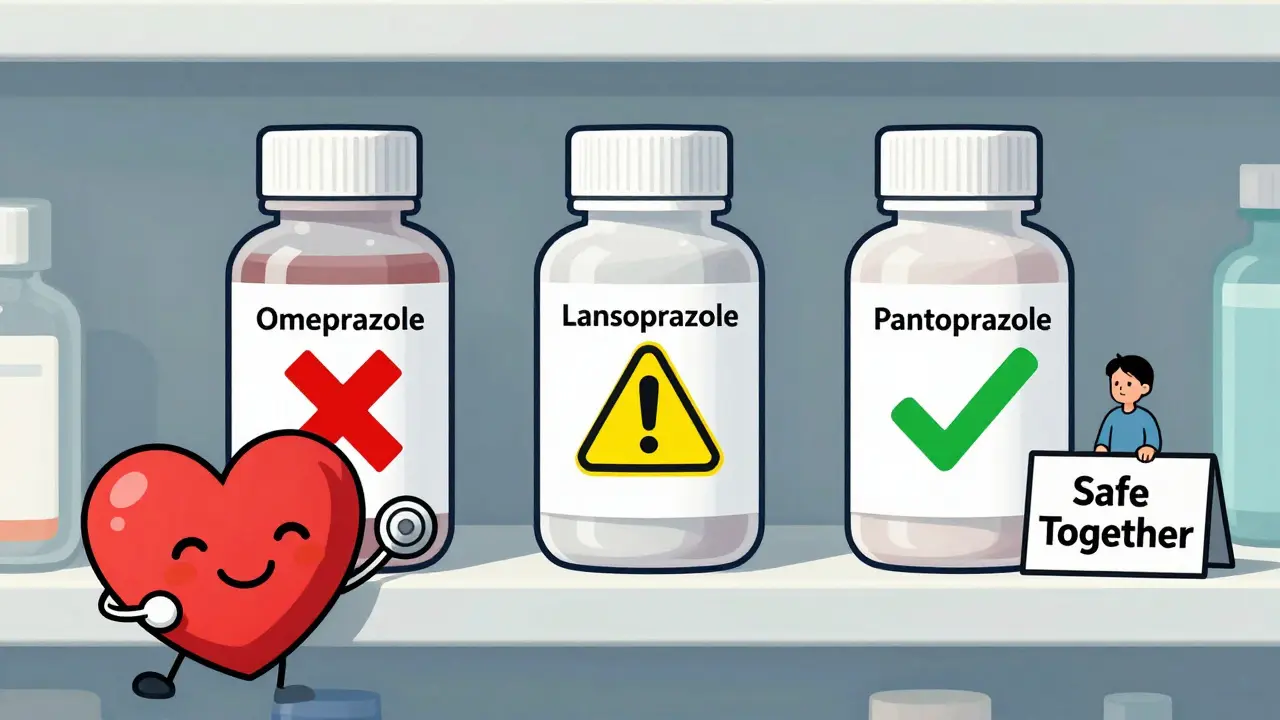
That’s why experts now say: if you need a PPI, don’t reach for omeprazole. Pantoprazole and dexlansoprazole are much safer choices. They barely touch CYP2C19. In fact, a 2024 study in JAMA Network Open found pantoprazole had no significant effect on clopidogrel’s ability to prevent clots - even at doses four times higher than normal.
Who’s Most at Risk?
It’s not just about which PPI you take. Your genes matter too. About 30% of people have a genetic variation that already makes CYP2C19 less effective. These are called loss-of-function alleles - mostly the *2 and *3 variants. If you carry one or two of these, your body naturally produces less of clopidogrel’s active form. Add omeprazole on top, and you’re at double risk.People with these gene variants have a 53% higher chance of major heart events, according to a landmark 2009 study in the New England Journal of Medicine. That’s why some hospitals now offer genetic testing for patients on clopidogrel - especially those with stents, diabetes, or prior heart attacks. The test costs between $350 and $500, and while it’s not routine everywhere, it’s becoming more common in high-risk clinics.
What Do Guidelines Say?
The advice isn’t the same everywhere. In the U.S., the American College of Cardiology and American Heart Association updated their 2023 guidelines to say: if you need a PPI, use pantoprazole or dexlansoprazole. They don’t say to avoid all PPIs - because the risk of a bleeding stomach ulcer is real. In fact, dual antiplatelet therapy (clopidogrel + aspirin) increases your risk of GI bleeding by 50%. A PPI can cut that risk in half.But in Europe, the European Society of Cardiology is stricter. Their 2023 guidelines recommend avoiding omeprazole and esomeprazole entirely when taking clopidogrel. The FDA still has a black box warning on clopidogrel’s label: "Avoid concomitant administration of omeprazole or esomeprazole."
So why the difference? It comes down to how each group weighs the evidence. Some experts believe the interaction is real and dangerous. Others argue that real-world data doesn’t show a big spike in heart events - even with omeprazole. Dr. Marc Cohen, who led the COGENT trial, says the GI protection from PPIs outweighs the tiny risk of reduced clopidogrel effect. But Dr. Deepak Bhatt, who studied stent thrombosis, points to clear increases in clots when omeprazole is used.
What Should You Do?
If you’re taking clopidogrel and a PPI, here’s what to ask your doctor:- Which PPI am I on? If it’s omeprazole or esomeprazole, ask if switching to pantoprazole or dexlansoprazole is an option.
- Do I have any risk factors for poor clopidogrel response? (Age over 65, history of ulcers, diabetes, kidney disease)
- Have I been tested for CYP2C19 gene variants? If not, is testing right for me?
- If I can’t switch PPIs, should I take clopidogrel at night and the PPI in the morning? This can help reduce competition for the enzyme.
One thing to remember: don’t stop your PPI without talking to your doctor. Stopping it could lead to a bleeding ulcer - which is just as dangerous as a clot.
The Bigger Picture: Cost, Access, and Future Drugs
There’s a financial side to this too. In the U.S., generic omeprazole costs about $0.38 per pill. Pantoprazole? Around $1.27. For Medicare patients, that’s an extra $147 a year. Many pharmacies still stock omeprazole as the default because it’s cheaper - even though guidelines say not to use it with clopidogrel.And here’s the future: newer antiplatelet drugs like ticagrelor and prasugrel don’t rely on CYP2C19. They work directly. But they’re expensive - ticagrelor costs over $500 a month. For many, clopidogrel remains the only affordable option. That means this interaction isn’t going away.
Even more concerning, a 2024 study in Circulation Research found that PPIs themselves may reduce nitric oxide - a molecule that helps blood vessels relax. That could mean PPIs might have independent heart risks, separate from clopidogrel. More research is needed, but it adds another layer to the conversation.
Bottom Line
You don’t have to choose between a heart attack and a bleeding ulcer. There’s a middle ground. If you’re on clopidogrel and need a PPI, ask for pantoprazole or dexlansoprazole. Avoid omeprazole and esomeprazole. If you’re already on them, don’t panic - but do talk to your provider. Your next prescription could be a simple switch that keeps you safer.Can I take omeprazole with clopidogrel if I take them at different times of day?
Taking clopidogrel at night and omeprazole in the morning may reduce the interaction slightly, but it doesn’t eliminate it. Studies show CYP2C19 inhibition is still significant even with staggered dosing. The best approach is to switch to a safer PPI like pantoprazole rather than relying on timing.
Is pantoprazole really safe with clopidogrel?
Yes. Multiple large studies, including the COGENT trial and a 2024 JAMA Network Open analysis, show pantoprazole has minimal to no effect on clopidogrel’s antiplatelet activity. It’s the preferred PPI in both U.S. and European guidelines for patients on clopidogrel.
Should I get genetic testing for CYP2C19?
It’s not needed for everyone. But if you’ve had a stent, a heart attack, or a clot despite being on clopidogrel, testing may help. If you’re a heavy smoker, have diabetes, or are over 70, you’re already at higher risk - and testing can guide whether you should switch to ticagrelor instead.
Why do some doctors still prescribe omeprazole with clopidogrel?
Cost, habit, and lack of awareness. Omeprazole is cheaper and widely available. Some doctors haven’t kept up with the latest guidelines. Others believe the risk is too small to matter. But for patients with multiple risk factors, the consequences can be serious.
Are there any natural alternatives to PPIs for stomach protection?
H2 blockers like famotidine or ranitidine (if available) can be used in some cases, but they’re less effective than PPIs at preventing serious GI bleeding. Antacids only help temporarily. There’s no natural substitute that matches the protection a PPI provides for high-risk patients. Don’t replace a prescribed PPI with supplements without medical advice.
14 Comments
Allison Priole
March 20 2026
okay so i read this whole thing and honestly? i’m just glad i’m not the only one who’s confused.
my doc put me on clopidogrel after my stent and then threw in omeprazole like it was nothing. i didn’t even know there was a problem until my cousin (who works at a hospital) asked me if i was taking ‘that stomach med’ with my heart med.
so i switched to pantoprazole last week and honestly? no difference in my stomach. no weird side effects. no drama. just… less panic.
also i didn’t get tested for genes because my insurance said no. so i just did the cheapest safe swap. and now i feel like a hero. 🙌
ps. if you’re on clopidogrel and your PPI is omeprazole? just ask. no shame. we’re all just trying not to die.
Casey Tenney
March 22 2026
People are dying because doctors still prescribe omeprazole with clopidogrel. That’s not a ‘gray area.’ That’s negligence.
Stop pretending this is a ‘cost issue.’ It’s a failure of education.
And if you’re one of those ‘it’s not that bad’ people? You’re part of the problem.
Timothy Olcott
March 22 2026
OMG YES 😤
My uncle had a stent. Took omeprazole. Had another heart attack 6 months later. Docs said ‘coincidence.’
Turns out? It wasn’t.
USA needs to wake up. This isn’t politics - it’s survival.
Switch your PPI. Now. 🇺🇸🩺
Paul Cuccurullo
March 23 2026
It’s remarkable how often we treat medicine like a puzzle with one correct answer, when in reality, it’s a balancing act of risk, access, and human behavior.
Yes, pantoprazole is preferred. Yes, omeprazole carries risk. But we cannot ignore the fact that thousands of patients - particularly those without resources - are still on omeprazole because it’s the only option they can access.
Instead of shaming clinicians who prescribe it, we should be advocating for policy changes that make safer alternatives universally affordable.
Knowledge without equity is just another form of elitism.
Bryan Woody
March 25 2026
Let me break this down like I’m explaining it to my grandma who still thinks ‘if it’s generic, it’s the same’
Clopidogrel = your body’s bouncer at the club. It keeps platelets from crashing the party.
Omeprazole = the bouncer’s cousin who shows up drunk and starts blocking everyone - even the ones who should be let in.
Pantoprazole? The bouncer’s chill roommate who just nods and says ‘cool, I’ll handle the door.’
So yeah. Switch. Not because it’s ‘trendy.’ Because your heart doesn’t care about your pharmacy’s profit margin.
Also - genetic testing? If you’re over 65, diabetic, and had a stent? You’re already in the high-risk club. Stop waiting for permission. Ask for the test.
And if your doctor says ‘we’ve always done it this way’? Smile. Then find a new one.
This isn’t complicated. It’s just inconvenient for the system.
Chris Dwyer
March 26 2026
Hey - if you’re reading this and you’re on clopidogrel + omeprazole? First - breathe.
You’re not alone. You’re not stupid. You didn’t mess up.
Now - next time you see your doctor, say: ‘Can we talk about switching my PPI?’
That’s it. No guilt. No panic. Just a simple question.
And if they say ‘no’? Ask why. Ask if pantoprazole is an option. Ask if your pharmacy can order it.
You’ve survived a heart attack. You can handle this conversation.
I believe in you. 💪
Desiree LaPointe
March 26 2026
Oh honey. You mean to tell me that after 20 years of medical science, we’re still playing ‘which PPI is the least evil’? How quaint.
Meanwhile, in the real world, patients are being sold $1,200/month ticagrelor while their doctors quietly refill their omeprazole script because ‘it’s what the patient’s used to.’
And yes - I know the guidelines say ‘pantoprazole.’ But have you seen the price tag? Or the fact that 80% of pharmacies don’t even stock it as the default?
Let’s not pretend this is about science.
This is about capitalism masquerading as clinical decision-making.
And if you’re still prescribing omeprazole? You’re not ignorant. You’re complicit.
Jackie Tucker
March 26 2026
How ironic that we’ve elevated ‘evidence-based medicine’ to a religion - yet ignore the most obvious truth: drugs don’t live in a vacuum.
The CYP2C19 interaction is real. But so is the fact that patients die from GI bleeds if you remove PPIs. So we’ve created a false binary: ‘safe PPI’ vs. ‘dangerous PPI.’
What we really need is a paradigm shift: move away from clopidogrel entirely.
Why are we clinging to a 20-year-old prodrug when ticagrelor exists? Because cost. Because inertia. Because we’re afraid of the future.
And until we stop treating patients like cost centers, we’ll keep patching the same leak with different tape.
Thomas Jensen
March 28 2026
Wait…
What if the whole thing is a pharmaceutical scam?
I mean - who profits from switching PPIs? The big pharma companies that make pantoprazole and dexlansoprazole.
And who gets left behind? The poor folks who can’t afford the upgrade.
And what about that 2024 Circulation study saying PPIs reduce nitric oxide? That’s not just about clopidogrel - that’s about heart health on its own!
Are we being manipulated into thinking this is a ‘drug interaction’ when it’s really a profit-driven replacement?
And why is nobody talking about how the FDA black box warning was added in 2009… and then quietly ignored?
Something’s off here. I’m not paranoid. I’m informed.
matthew runcie
March 28 2026
Switched to pantoprazole last month. No issues. No drama. Just peace of mind.
My doctor didn’t mention the interaction. I read it online. Then asked. He said ‘good catch.’
Simple. Effective.
Thanks for the clarity.
Shaun Wakashige
March 28 2026
lol just switch to famotidine. cheaper. same effect. no interaction.
problem solved. 🤷♂️
Johny Prayogi
March 29 2026
Just got my genetic test back - I’m a slow metabolizer. Omeprazole was killing my clopidogrel.
Switched to pantoprazole. No more chest tightness. No more panic.
My doc was shocked I even knew to ask. Thanks to this post - I’m alive.
Everyone reading this - if you’re on clopidogrel, ask. Just ask.
You’ve got this. 💙
Sandy Wells
March 30 2026
Replying to @matthew runcie: you’re right. But famotidine? It’s not as good at preventing bleeding ulcers as PPIs. Especially in high-risk patients on dual antiplatelet therapy.
And it wears off faster. You’re trading convenience for incomplete protection.
It’s a band-aid. Not a solution.






Sandy Wells
March 20 2026
So let me get this straight - we’re telling people to swap a $0.38 pill for a $1.27 pill just to avoid a theoretical risk that might not even show up in real-world data? I’ve seen patients bleed out because their PPI got switched and they didn’t get the follow-up. This feels like guideline theater.
Also - who’s paying for dexlansoprazole when the insurance won’t cover it? Real talk: if you’re on Medicare and can’t afford the difference, you’re stuck with omeprazole. No amount of JAMA studies changes that.
And don’t even get me started on genetic testing. $500 to find out you’re a slow metabolizer? Meanwhile, the guy next to you in the ER got a stent and got discharged with omeprazole because his doctor didn’t know any better. This system is broken.
I’m not saying don’t switch. I’m saying stop pretending this is a clean, easy fix. It’s not. It’s a patchwork of privilege, cost, and ignorance.
Also - why is everyone acting like pantoprazole is magic? It’s still a PPI. Long-term use = vitamin B12 deficiency, kidney issues, bone fractures. We’re trading one risk for another. And nobody talks about that.
Just say it: we need better drugs. Not better timing. Not better pills. Better drugs.
And if you’re still prescribing omeprazole? You’re not a bad doctor. You’re just working in a broken system.
But yeah. I still think we’re overcomplicating it.